Translate this page into:
Pseudomonas infection of nail: Green nail syndrome secondary to onychomycosis

*Corresponding author: Department of Dermatology, All India Institute of Medical Sciences Rishikesh, Rishikesh, Uttarakhand, India. anmolbatra9@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Batra A, Hazarika N. Pseudomonas infection of nail: Green nail syndrome secondary to onychomycosis. CosmoDerma 2022;2:55.
A 21-year-old female presented with a 3-month history of slowly progressive greenish-black discoloration of right middle fingernail and left ring fingernail, with distolateral onycholysis of both middle fingernails and left ring fingernail with proximal nontender paronychia of both middle fingernails [Figure 1]. There was mild pus discharge from undersurface of left middle fingernail as well.
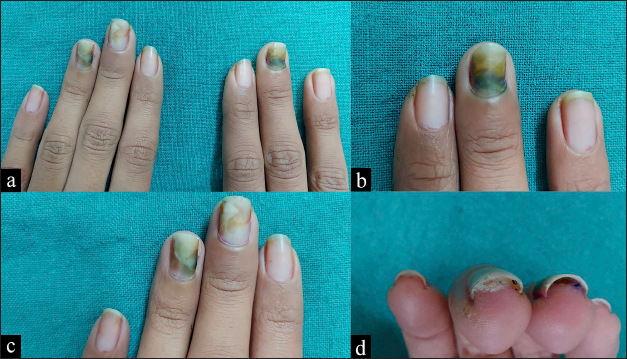
- Proximal greenish-black discoloration, distolateral onycholysis, and proximal paronychia seen over (a) both middle fingernails and left ring fingernail. (b) Close-up view of right middle fingernail. (c) Close-up view of left middle and ring fingernail. (d) Mild pus discharge from undersurface of left middle fingernail.
Direct mycologic examination of nail scrapings was positive for fungal elements and bacteriologic examination of nail scrapings revealed Pseudomonas aeruginosa infection. She was prescribed itraconazole 200 mg/day 7 days per month for 2 months for fungal infection and oral ciprofloxacin 500 mg/day for 3 weeks for pseudomonas coverage. There was significant improvement on follow-up.
P. aeruginosa is the most common pathogen causing bacterial nail infections.[1] Treatment options include topical gentamicin for 1-3 months or oral ciprofloxacin for 2-3 weeks.
Declaration of patient consent
Patient’s consent not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Infections of finger and toe nails due to fungi and bacteria. Hautarzt. 2014;65:337-48.
- [CrossRef] [PubMed] [Google Scholar]





