Translate this page into:
Mitten glove deformity - A marker of dystrophic epidermolysis bullosa

*Corresponding author: Anubhab Bhattacharyya, Department of Dermatology, Jawaharlal Institute of Postgraduate Medical Education and Research, Puducherry, India. anubhabriorik@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Bhattacharyya A, Rout N. Mitten glove deformity - A marker of dystrophic epidermolysis bullosa. CosmoDerma 2023;3:140.
A 10-year-old boy, firstborn to a non-consanguineous marriage, came with recurrent blistering since birth, particularly over the trauma-prone areas of the body. The blisters would leave behind areas of ulceration, which heal with significant atrophic scarring, depigmentation, and milia formation. The scarring is to such an extent as to cause significant functional impairment in the form of contractures across joints (marked over the interphalangeal joints of the hands and feet and the knee joint) and difficulty in opening the mouth. Recurrent episodes of ulceration and scarring have finally resulted in an intact cocoon of skin that completely encases most of the digits of the hands and feet [Figure 1a-f]. The fingers were attached to each other as well as to the palms [Figure 1d and e] – only the right thumb was relatively free and capable of independent movements. Such characteristic appearance is also known as pseudosyndactyly or “Mitten Glove deformity” – which has been classically described in recessive dystrophic epidermolysis bullosa (RDEB).[1]
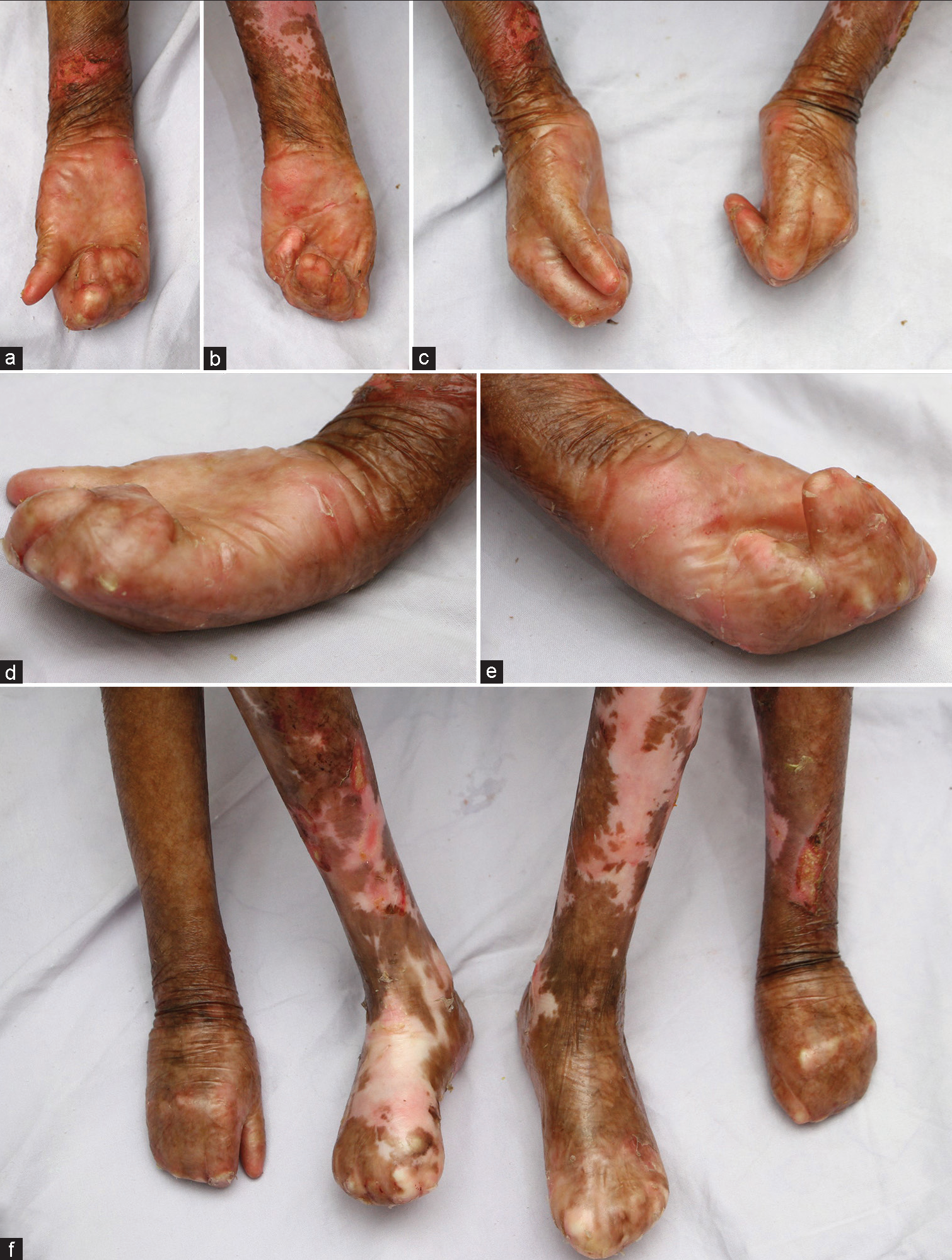
- Anterior view (a and b) and lateral view (c) of bilateral hands showing fusion of digits to each other imparting the “mitten glove appearance”. Lateral view (c) shows the relatively free the right thumb. Views (d and e) depict the side profile of the hands showing fusion of digits to palms. The anteroposterior view of hands and feet (f) demonstrate scarring, depigmentation and pseudosyndactyly.
RDEB is an inherited bullous disorder resulting from the congenital absence of or defective collagen VII protein, thus causing the weakened sublamina densa region of the basement membrane zone to yield under shearing forces and to cause ulcers that heal with scarring and milia. Cutaneous scarring in dystrophic epidermolysis bullosa may lead to a variety of complications, particularly joint contractures and fusion of the fingers and toes.[1] Progressive hand deformity is common in more severe forms of RDEB. Timely and sterile rupture of bullae followed by non-adhesive dressing over them, particularly in between the fingers, can help to prevent the formation of scar in the first place. In case of already established mitten glove deformity, surgical corrective procedures such as transverse release procedures can also be undertaken. Thus, the presence of such clinical findings can thus be used to aid in the diagnosis of RDEB.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Epidermolysis bullosa In: Harper’s textbook of pediatric dermatology. Vol 118. United States: John Wiley & Sons, Ltd.; 2011. p. :1-34. Available from: https://onlinelibrary.wiley.com/doi/abs/10.1002/9781444345384.ch118 [Last accessed on 2023 Sep 20]
- [CrossRef] [Google Scholar]





