Translate this page into:
Decoding eczematous lesions occurring post-surgery

-
Received: ,
Accepted: ,
How to cite this article: Narayanan A, Ram Kumar KR, Kotekar S, Krishna J, Thappa DM. Decoding eczematous lesions occurring post-surgery. CosmoDerma 2022;2:29.
Dear Sir,
Surgical procedures can result in a broad spectrum of cutaneous changes. Eczematous lesions at surgical sites include autonomic denervation dermatitis, post-traumatic eczema, and “surgery of the knee, injury to the infrapatellar branch of the saphenous nerve, traumatic eczematous dermatitis (SKINTED).” We describe two patients presenting with postsurgical eczema.
CASE 1
A 45-year-old male patient presented with itchy, hyperpigmented, scaly eczematous plaques with oozing and excoriations over the left medial aspect of the left distal leg Figure 1a for 6 months. The patient was a known diabetic on regular treatment. He was involved in a road accident 2 years ago, resulting in his right little toe amputation. He had undergone skin graft transfer from the left distal part of the leg to the right foot [Figure 1b]. The patient started developing eczematous lesions over the graft site 1.5 years later. There was a moderate sensory deficit to touch and pain. We made a final diagnosis of autonomic denervation dermatitis based on the history. We treated our patient with topical corticosteroids with good improvement.
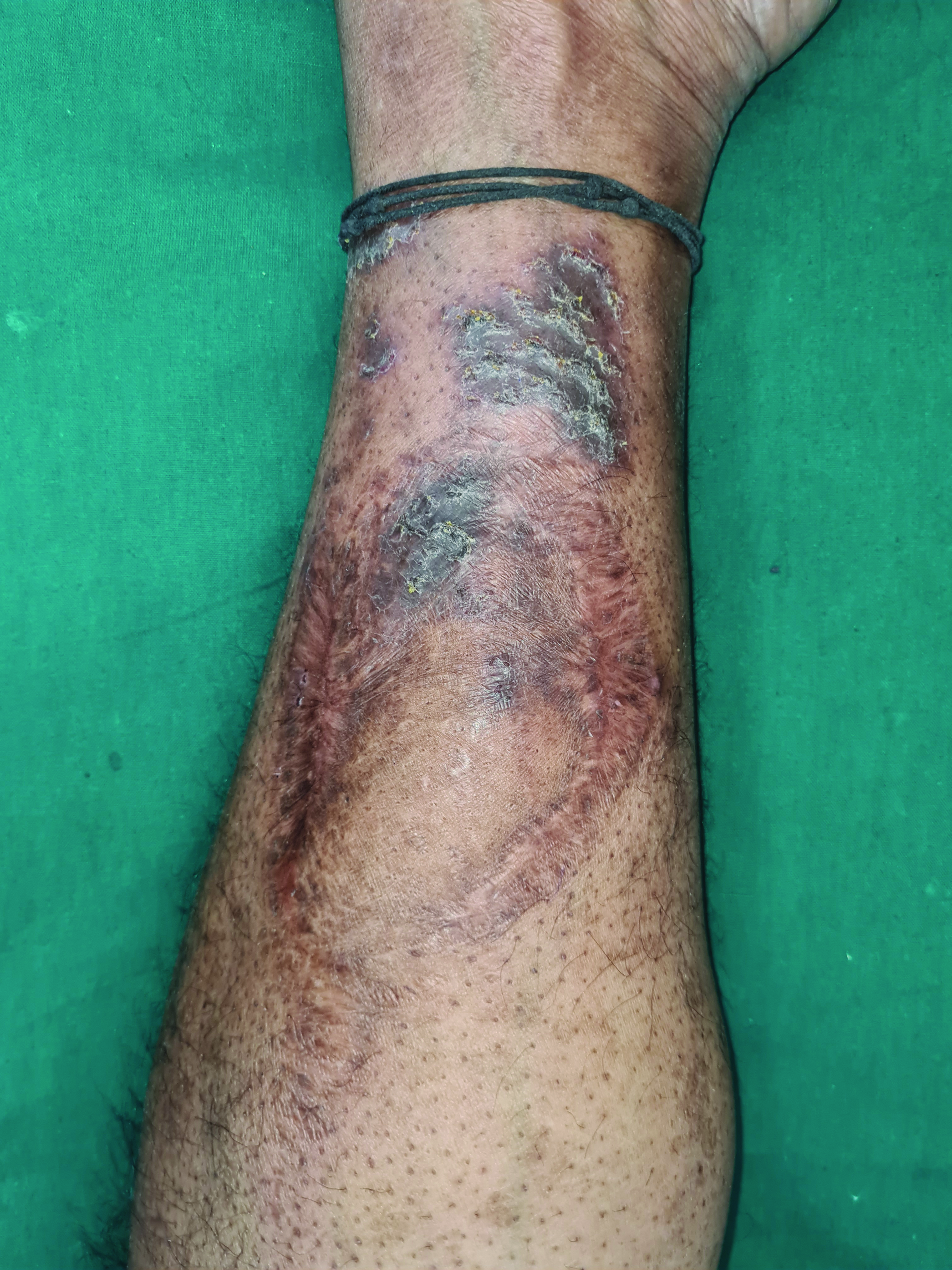
- Hyperpigmented, scaly eczematous plaque with oozing and excoriations over the left medial aspect of left distal leg
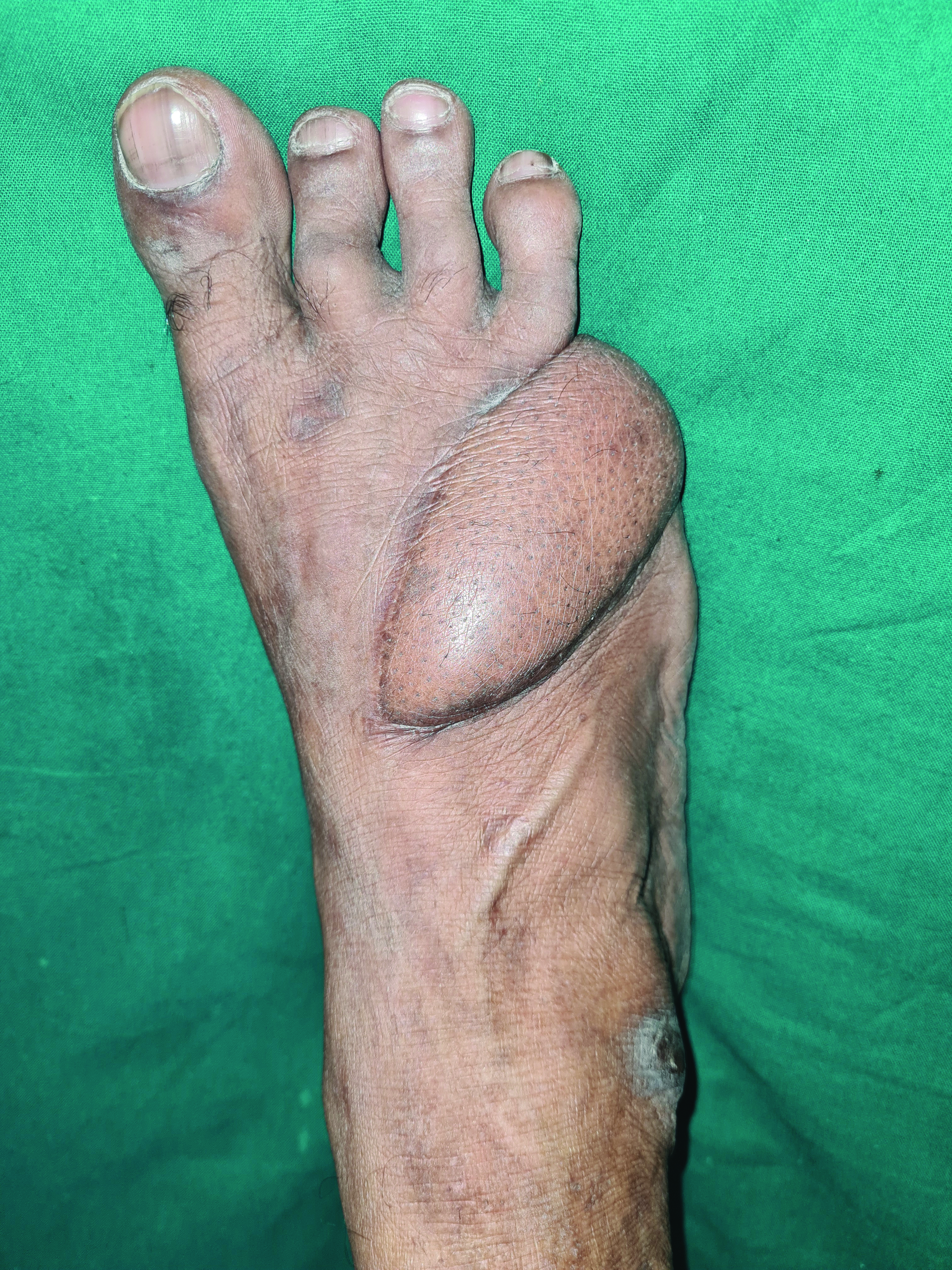
- Skin graft site over the right foot
CASE 2
A 62-year-old female patient with itchy, hyperpigmented, scaly eczematous plaques linearly distributed along the medial aspect of the left leg [Figure 2]. The patient had undergone a saphenous vein graft as a part of coronary artery bypass graft two years ago. She started developing eczematous lesions from where a saphenous vein graft was taken 6 months after surgery. The patient had minimal sensory deficit over the incision scar. We made a final diagnosis of autonomic denervation dermatitis and treated it with topical corticosteroids with good improvement.
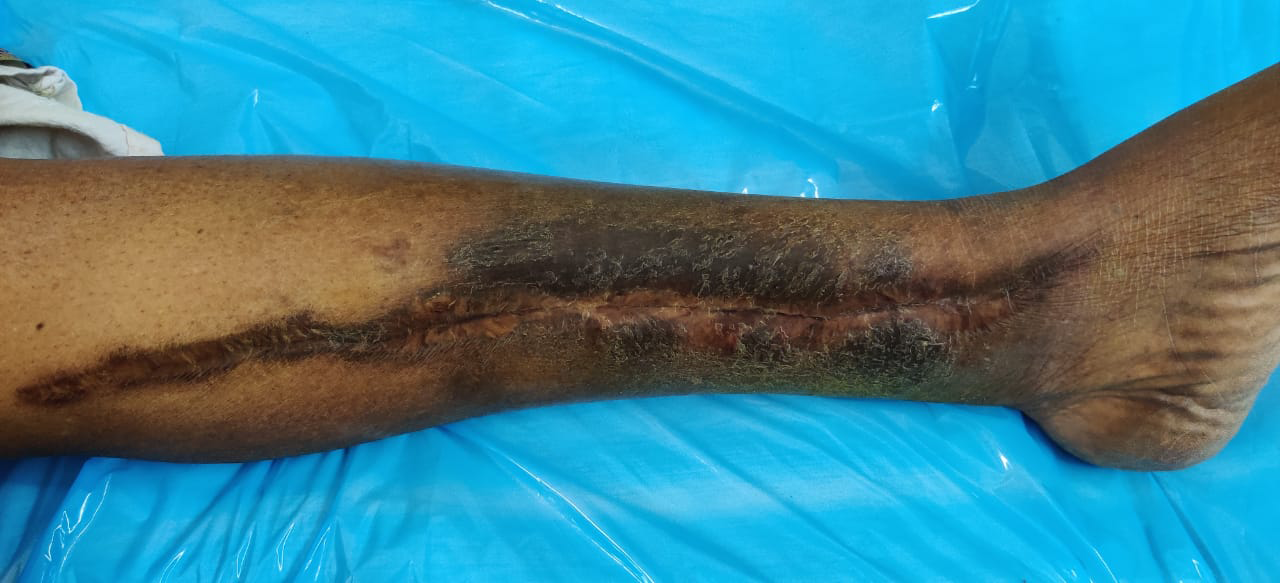
- Hyperpigmented, scaly eczematous plaque linearly distributed along the medial aspect of the left leg
Autonomic nerve fibers play an important role in sweat gland function, vasomotor activity, and cutaneous blood flow. The skin barrier function is maintained by the normal functioning of sweat glands, sebaceous glands, and cutaneous blood flow. Impaired sudomotor activity has a role in the development of dermatitis. Acetylcholine and catecholamines secreted from autonomic nerve endings modulate keratinocyte proliferation, adhesion, migration, and differentiation. During nerve regeneration, there is a release of neuropeptides from nerve terminals during nerve regeneration. The neuropeptides, including substance P, calcitonin gene-related protein, vasoactive intestinal peptide, and neurotensin, modulate the presentation of epidermal antigen. They also play a role in immediate and delayed-type hypersensitivity reactions resulting in dermatitis.
Cutaneous surgeries result in traumatic damage to dermal nerve fibers. This nerve damage results in the denervation of various autonomic organs of the skin. The altered cutaneous anatomy and physiology following autonomic nerve injury is termed “trophoneurosis.” Verma and Mody described “surgery of the knee, injury to the infrapatellar branch of the saphenous nerve, traumatic eczematous dermatitis (SKINTED).”[1] The condition was region and procedure-specific. It occurs 3 weeks to 4 months after knee surgery. The condition was accompanied by hypoesthesia/anesthesia, which develop soon after surgery and resolved once the skin lesions appeared.[2] Mathias proposed the term “post-traumatic eczema.”[3] Sharquie et al. proposed “neuropathy dermatitis” to describe eruptions similar to SKINTED.[4] Madke recently suggested the term “autonomic denervation dermatitis.”[5] Table 1 lists the differences between autonomic denervation dermatitis, post-traumatic eczema, and SKINTED.
| Clinical features | Autonomic denervation dermatitis | Post-traumatic eczema | SKINTED |
|---|---|---|---|
| Onset | Months to years after surgery | 3-4 weeks after trauma | Months to years after surgery to the knee |
| Nature of trauma | Surgery | Mechanical/ thermal/ chemical trauma | Knee surgery |
| Site | At surgical site | At traumatic site | Surgical site over knee |
| Nature of wound | Healed surgical site | Wound in healing phase | Healed surgical site |
| Recurrent | Persistent/ recurrent lesions | Recurrent lesions | Recurrent lesions |
Post-traumatic eczema occurs 2-4 weeks after mechanical, thermal, or chemical injury. The lesions occur in and around the wound, often during healing. The pathogenesis of post-traumatic eczema includes atopic predisposition and post-traumatic inflammatory response (koebnerization).[5] The condition frequently recurs over multiple years.
Autonomic denervation dermatitis presents with xerosis and anesthesia/hypoesthesia months to years after surgical trauma,[6] after the surgical site has healed [Table 2]. Autonomic denervation dermatitis results from transection of dermal nerves during cutaneous surgery.[7] The lesions of autonomic denervation dermatitis are persistent or recurrent. Patients often present with relapses in winters and should be counselled regarding the chronic nature of the disease.[8] SKINTED is a site and procedure specific subset of autonomic denervation dermatitis.
| Author | Age | Gender | Time lag between surgery and development of ADD | Nature of trauma | Site | Clinical features |
|---|---|---|---|---|---|---|
| Madke et al. 5 | 60 | F | 10 months | Total knee replacement | Left knee | Eczematous, scaly, oozy lesion |
| Madke et al. 5 | 58 | M | 18 months | Saphenous vein graft harvest | Medial aspect of right leg | Dry, scaly, ill-define lesion |
| Madke et al. 5 | 59 | M | 2 years | Total knee replacement | Right knee | Dry, scaly, pruritic lesions |
| Madke et al. 5 | 49 | M | 6 months | Saphenous vein graft harvest | Medial aspect of right leg and ankle joint | Eczematous lesion with dry skin |
| Madke et al. 5 | 59 | M | 1 year | Total knee replacement | Left knee | Pruritic, oozy papulovesicular lesion |
| Madke et al. 5 | 55 | M | 1 year | Saphenous vein graft harvest | Right leg and ankle | Eczematous lesion |
| Madke et al. 5 | 55 | M | 2 years | Open reduction and internal fixation of femur fracture | Lateral aspect of right thigh | |
| Madke et al. 5 | 60 | M | 3 years | Saphenous vein graft harvest | Right leg and ankle joint | Eczematous lesion |
| Madke et al. 5 | 61 | M | 9 months | Total knee replacement | Left knee | Oozy, papulovesicular lesion |
| Madke et al. 5 | 65 | M | 2 years | Total knee replacement | Right knee | Oozy papulovesicular lesion |
| Mathur et al. 8 | 70 | M | 1 year 4 months | Bilateral total knee replacement | Bilateral knees | Itchy, dry lesions |
| Mathur et al. 8 | 49 | F | 11 months | Bilateral total knee replacement | Bilateral knees | Itchy, red lesions |
| Pathania et al. 1 | 60 | F | 9 months | Bilateral knee replacement surgery | Bilateral knees | Oozy, red lesions on left knee Hyperpigmented, raised lesion on right knee |
| Bose et al. 6 | 48 | M | 6 months | Saphenous vein graft harvest | Right medial malleolus to upper thigh | Oozy, crusted lesion with xerosis |
| Biswas et al. 7 | 54 | M | 11 months | Saphenous vein graft harvest | Left leg | Red, oozy, lesions |
The presentation of post-traumatic eczema and autonomic denervation dermatitis are very similar. Dermatologists should be aware of the differences between these two entities to make a proper diagnosis.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- SKINTED: An autonomic denervation dermatitis. Int J Dermatol. 2020;59:613-4.
- [CrossRef] [PubMed] [Google Scholar]
- Explaining a hitherto nameless condition: ‘SKINTED’. Clin Exp Dermatol. 2009;34:e465-e466.
- [CrossRef] [PubMed] [Google Scholar]
- Idiopathic post-traumatic eczema. Contact Dermatitis. 2006;54:178.
- [CrossRef] [PubMed] [Google Scholar]
- Neuropathy dermatitis following surgical nerve injury. Case Rep Dermatol Med. 2011;2011:234185.
- [CrossRef] [PubMed] [Google Scholar]
- Autonomic denervation dermatitis: A new type of eczematous dermatitis. Clin Dermatol Rev. 2017;1:61-4.
- [CrossRef] [Google Scholar]
- Autonomic denervation dermatitis following saphenous vein grafting: A case report. Int J Dermatol 2021:34817854.
- [CrossRef] [Google Scholar]
- Autonomic denervation dermatitis in two patients. Indian J Clin Dermatol. 2019;2:96-7.
- [Google Scholar]





