Translate this page into:
Imatinib-induced pseudoheliotrope rash

*Corresponding author: Aravind Sivakumar, Department of Dermatology, JIPMER, Pudhucherry, India. aravinddermat@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Sivakumar A, Selvaraj R. Imatinib-induced pseudoheliotrope rash. CosmoDerma 2023;3:146.
A 32-year-old woman presented with asymptomatic hyperpigmentation surrounding the eyelids for 1-month duration. She was recently diagnosed with a case of gastrointestinal stromal tumor (GIST) and started on imatinib therapy. After 2 weeks of drug intake, she noticed edema of both eyelids which progressed to redness without any local symptoms after which the drug was stopped. There were no associated skin lesions elsewhere and no features of muscle weakness. On examination, well-defined violaceous symmetrical hyperpigmentation was noted over the bilateral upper and lower eyelids [Figure 1]. Investigations revealed normal levels of muscle enzymes (creatinine phosphokinase-total and MB, aspartate aminotransferase, lactate dehydrogenase). The patient was advised low potent topical steroid application over the area (hydrocortisone acetate 0.1%). There was marked improvement of the lesions after 1 week. The Naranjo score for adverse drug reaction was 6 suggesting probable drug reaction. Hence, imatinib-induced heliotrope-like eruption was considered.
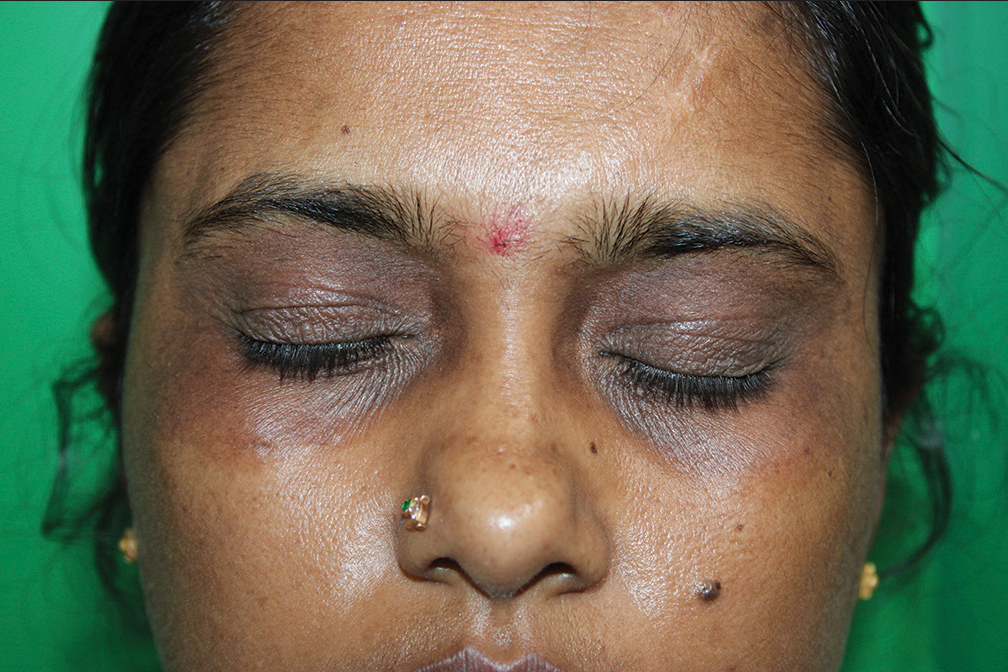
- Heliotrope-like rash noted over both eyelids.
The heliotrope rash is named after the purplish flowers of the plant Heliotropium arborescens which is derived from the Greek “helios,” meaning “sun,” and “trepein,” meaning “to turn.” The periorbital lilac-colored rash in dermatomyositis occurs due to the inflammation of the eyelid muscles underneath the thin skin of the eyelids. Imatinib is a tyrosine kinase inhibitor that is used for various malignancies such as chronic myeloid leukemia, myelodysplastic syndrome, GIST, and also for dermatological indications such as systemic mastocytosis, hypereosinophilic syndrome, Kaposi sarcoma, and dermatofibrosarcoma protuberans. It is associated with various cutaneous adverse events such as maculopapular rash, lichenoid eruption, vitiligo-like depigmentation, and hand-foot syndrome. Periorbital edema with heliotrope-like eruption occurs as a rare side effect of imatinib and needs to be distinguished from heliotrope rash of dermatomyositis. Other drugs causing dermatomyositis like skin changes include hydroxyurea, penicillamine, statins, cyclophosphamide, and anticonvulsants. Absence of muscle weakness and other cutaneous signs of dermatomyositis such as Gottron’s sign and papules, V sign, shawl sign, normal muscle enzymes, negative autoantibodies, and resolution following stoppage of drug favors pseudoheliotrope rash of imatinib. Histology cannot distinguish between heliotrope rash and heliotrope-like eruption which shows a lichenoid pattern of interface dermatitis in both these cases. Treatment is mainly conservative with topical steroids or calcineurin inhibitors.[1]
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Heliotrope-like eruption mimicking dermatomyositis in a patient treated with imatinib mesylate for chronic myeloid leukemia. Int J Dermatol. 2006;45:1249-51.
- [CrossRef] [PubMed] [Google Scholar]





