Translate this page into:
How I treat acne scars?

*Corresponding author: Rasya Dixit, Dr Dixit Clinic, 34, above HDFC bank, first main Koramangala 1st block Bangalore 560034, Karnataka, India. dr.rasya@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Dixit R. How I treat acne scars? CosmoDerma 2021;1:39.
Abstract
Acne scars affect up to 95% of those suffering from acne and have a significant negative effect on quality of life. It is imperative to complete acne treatment before scar treatment commences. The treatment of the scars begins with the analysis of the skin type, scar type, lifestyle, and sun exposure. Age of the patient, patient expectations, timelines, and budget are important considerations. Treatment of the scars includes release of the subdermal bands with subcision, improvement of the neocollagenosis by causing regular thermal or mechanical microinjury to the dermis, improvement of epidermal pigment, and improvement of skin hydration. Often, multiple treatments and multimodality treatments need to be used to give satisfactory results.
Keywords
Acne
Scars
Treatment
In an increasingly virtual world, the face holds the key to a confident first impression. Acne is a common condition and is now made increasingly so, by the addition of stress, lifestyle, and diet choices as well as decreasing ability to exercise due to restricted movement due to current COVID limitations. Post-acne scarring has been noted in up to 95% of patients with acne and is related to severity as well as delay in seeking treatment.[1] There is a definite negative effect on quality of life in patients affected by acne scars, which affects their psychosocial well-being.[1]
The primary step before starting the scar treatment is the prevention of further acne. I do emphasize the need for completion of treatment of acne, with medication as well as diet, exercise, and lifestyle modification. The patient has to be counseled to help understand the same; and the patients with acne should also be alerted that long-standing acne leads to scarring, and counseled about compliance to treatment.
The first consultation for the treatment of acne scars is to determine the duration of acne and scars, the treatment for acne and scars done, the skin type (both Fitzpatrick and Robert’s skin type), the type of acne scarring (macular, hypertrophic, ice-pick, rolling, or boxcar), age of the patient, motivation of the patient to seek treatment, patient expectations, as well as budget. All these will have an impact on the treatment plan, treatment duration, and end results as well.
The treatment plan needs to address the concerns of the patient keeping in mind the limitations of skin type, time, and budget. The expected outcome has to be explained to the patient, always under promise and over deliver is my mantra. The patient counseling to make sure they understand the procedure, the complications and the cost is important. Written informed consent is mandatory before starting treatment. Good photographs from different angles with standardized lighting are imperative at the start of treatment and before every session to see the progress. I also recommend a pre-treatment regime of broad-spectrum sunscreens in the daytime, a retinol, and non-hydroquinone-based skin lightening cream at night for at least 2 weeks before starting treatment to prevent post-inflammatory hyperpigmentation.
The release of the fibrous strands that anchor the scars usually forms the first treatment. This allows us to follow up with collagen regeneration treatments. My preferred method of subcision is to do a bilevel subcision with a blunt 22 G cannula at a deeper layer and a 26 G needle just below the skin. This allows me to get a good improvement at both the layers without any large bruise or hematoma formation that can be distressing to the patient.[2] I often combine the second step of collagen improvement treatment with this treatment, and repeat the subcision monthly at least 2–3 times to get the desired results.
Once the adherent fibrous strands are released, we start the treatments to induce collagen. This can be achieved by dermaroller/dermapen, fractional CO2 laser, or fractional microneedle radiofrequency treatment. The advantage of the dermaroller is low cost, lower chances of post-inflammatory hyperpigmentation, and lower downtime, however, the results tend to be mild to moderate and plateau faster. Fractional CO2 laser has an advantage of fewer consumables, however, a longer downtime as well higher chance of post-inflammatory hyperpigmentation should be considered, especially in darker skin types. This makes fractional microneedle radiofrequency a good treatment choice in many of my patients, as it combines the advantage of lower downtime and lesser post-inflammatory hyperpigmentation, however, consumable tip cost and slightly increased pain are the drawbacks.[3] Recent studies have shown the combination of these two technologies on the same session gives better results, and this multimodality treatment has been tried at our clinic for patients who do not respond adequately to any one modality. Treatments are done once a month, results are usually appreciable after the second session. Platelet-rich plasma injections are often combined with these treatments to reduce downtime and improve results.[4]
Open pores and ice-pick scars need special attention, being poor responders to treatment. I prefer multiple sessions of TCA CROSS to target these scar types.
Post-inflammatory hyperpigmentation and erythema can present along with acne scars, and can cause severe distress to the patient. Chemical peels such as salicylic peel, retinol peels, and Q switched Nd: YAG lasers can be used in combination with the topical treatments to help reduce the pigmentation.
An addition of a hyaluronic acid filler to the end of the treatment will significantly improve outcome as it improves the texture and hydration of the skin. The hyaluronic acid chosen is a moderate to low G prime product which can be placed under the scars as well as over areas of volume loss which may be seen in severe acne scars. It is best to combine this procedure with a bilevel subcision at the same session or 1 week before the filler as it allows the filler to be deposited easily under the scars [Figures 1 and 2]. This treatment can be offered as a standalone treatment for those patients who desire immediate improvement.[5]
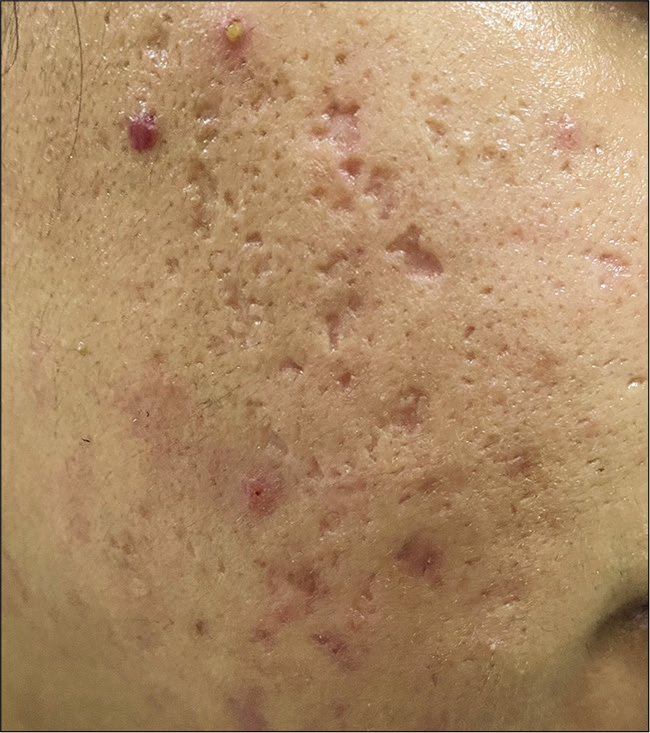
- Before treatment.
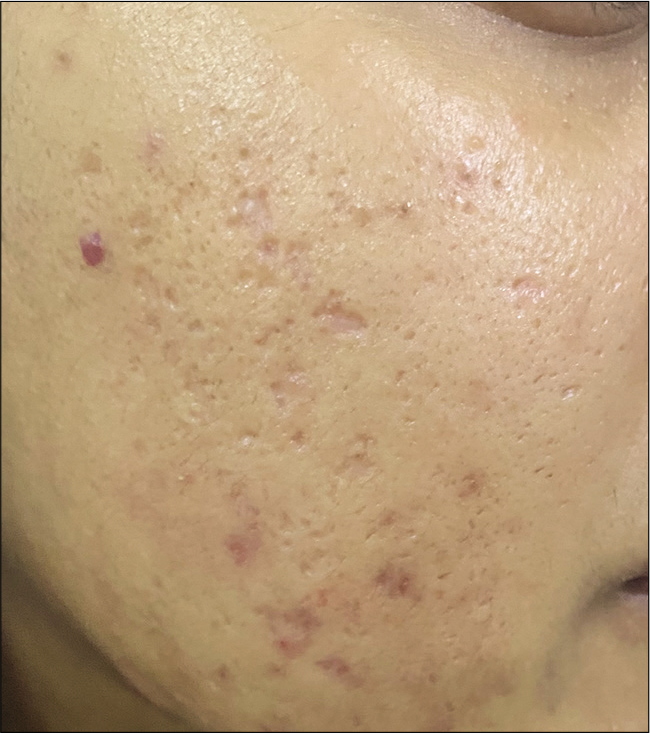
- After bilevel subcision and hyaluronic acid filler.
The most common complication is post-inflammatory hyperpigmentation. This can be avoided by use of sunscreen and topical skin lightening creams. Keeping treatment parameters, optimal and widening the intervals between treatments help to keep chances of side effects low.
Acne scars are a common outpatient complaint, and patients are aware and ready for treatment. Treatments can be optimized to the patient, after considering scar, skin type, and patient factors. Treatments can be gratifying to both patient and dermatologist.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Acne and acne scarring-the case for active and early intervention. Aust Fam Physician. 2006;35:503-4.
- [Google Scholar]
- Blunt cannula subcision is more effective than Nokor needle subcision for acne scars treatment. J Cosmet Dermatol. 2019;18:192-6.
- [CrossRef] [PubMed] [Google Scholar]
- Safety of combined fractional microneedle radiofrequency and CO2 as an early intervention for inflammatory acne and scarring treated with concomitant isotretinoin. Dermatol Surg. 2020;46:e71-7.
- [CrossRef] [PubMed] [Google Scholar]
- Treatment of acne scars with PRP and laser therapy: An up-to-date appraisal. Arch Dermatol Res. 2019;311:643-6.
- [CrossRef] [PubMed] [Google Scholar]
- Effectiveness and safety of acne scar treatment with nonanimal stabilized hyaluronic acid gel. Dermatol Surg. 2018;44:S10-18002.
- [CrossRef] [PubMed] [Google Scholar]






