Translate this page into:
A giant white macule since birth – Uncommon presentation of a common entity

*Corresponding author: Anubhab Bhattacharyya, Department of Dermatology, JIPMER, Puducherry, India. anubhabriorik@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Bhattacharyya A, Somasundaram A, Biswas S. A giant white macule since birth – Uncommon presentation of a common entity. CosmoDerma. 2023;3:186. doi: 10.25259/CSDM_240_2023
We present the case of a 7-month-old male child brought to the outpatient department by his parents with complaints of a large patch of pale discoloration over the right half of the trunk noted since birth. It was non-progressive and did not involve any other sites. There was no similar history in the family. On clinical examination, we noted the presence of a single large, well-defined depigmented macule involving the right half of the trunk (both anteriorly and posteriorly) extending over onto the medial aspect of the right arm [Figure 1a]. Margins were well defined and serrated. The depigmented patch did not cross the midline, and there was no associated ipsilateral breast hypoplasia or presence of other pigmentary abnormalities. Based on the onset and examination findings of depigmented macule with serrated borders and pseudopod-like extensions [Figure 1a and b], we arrived at a diagnosis of nevus depigmentosus. Upon application of pressure with a glass slide (the vitropression test), the margins of the macule did not disappear – thus favoring our diagnosis over another close differential of nevus anemicus. Dermoscopic findings of subtle pigment network [Figure 2 - black arrow] and serrated border/pseudopod [Figure 2 - red arrow] further supported our diagnosis.[1] The possibility of congenital vitiligo was also ruled out due to the absence of family history,[2] lack of typical site involvement like perianal region,[3] and lack of progression of the margins.

- (a) Giant depigmented macule over the right half of the trunk, anteriorly extending up to midline and laterally over the medial aspect of arm. (b) Contiguous extension of the macule over the back of trunk; inset and arrow shows the serrated margins and “pseudopod” like extension of the macule (highlighting the area of back outlined by smaller box).
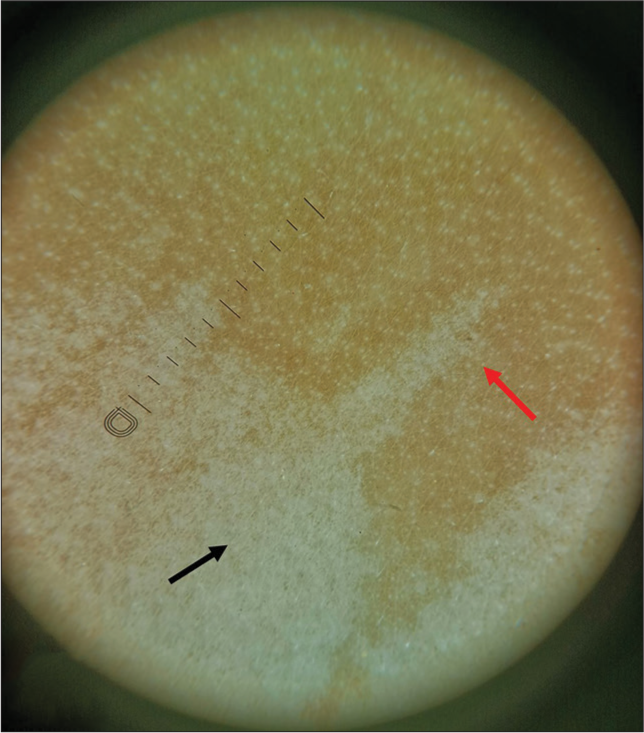
- Dermoscopy finding (Dinolite 4th Gen, ×10, polarized) serrated margin (red arrow), subtle pigmentary network (black arrow).
Nevus depigmentosus represents a condition wherein depigmentation (or hypopigmentation) exists as a solitary, localized macule or patch, sometimes existing in a Blaschkolinear fashion. While it is debated whether the condition is a form of mosaicism, it has generally been noted (in more than 90% of cases) that the onset is within the first three years of life, most often congenital.[4] Such lesions seldom progress or resolve by themselves. Cutaneous and extracutaneous associations that have been noted with this condition include – nevus spilus, nevus flammeus, Becker’s nevus, segmental lentiginosis, with ipsilateral breast hypoplasia, central nervous system involvement, and hemihypertrophy.[4] Treatment mostly is reassurance, surgical, and/or camouflage techniques.
Although nevus depigmentosus is not a rare clinical entity, we present here a case of a giant nevus depigmentosus unilateralis resembling a type 5 mosaicism (with lateralization), which has not been described much in literature, and at times, can be baffling to young dermatologists.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Congenital vitiligo: Time to think beyond the concept of acquired etiology. Indian J Paediatr Dermatol. 2016;17:328.
- [CrossRef] [Google Scholar]
- Harper's textbook of pediatric dermatology. United States: John Wiley & Sons; 2019:2536.
- [CrossRef] [Google Scholar]





