Translate this page into:
Giant tinea pseudoimbricata

*Corresponding author: Dr. Govind Srivastava, MBBS, MD, MNAMS, Skin Institute and School of Dermatology, Ashok Vihar, Delhi, India. sisdoctor@yahoo.co.in
-
Received: ,
Accepted: ,
How to cite this article: Srivastava G, Srivastava G. Giant tinea pseudoimbricata. CosmoDerma 2022;2:34.
A 9-year-old boy presented with a 6-month history of an itchy rash on the trunk. He was applying clobetasol cream for the past few months, yet the rash aggravated. On examination, two giant concentric annular lesions covering the chest and abdomen were visible. They were raised, erythematous, and scaly, enclosing an area of scaling and excoriation marks. Another similar lesion covered the lower abdomen and thighs [Figure 1]. Scraping from the active edge of the lesion revealed fungal hyphae under a microscope. A fungal culture on Sabouraud dextrose agar revealed Trichophyton rubrum. A diagnosis of tinea pseudoimbricata was made.
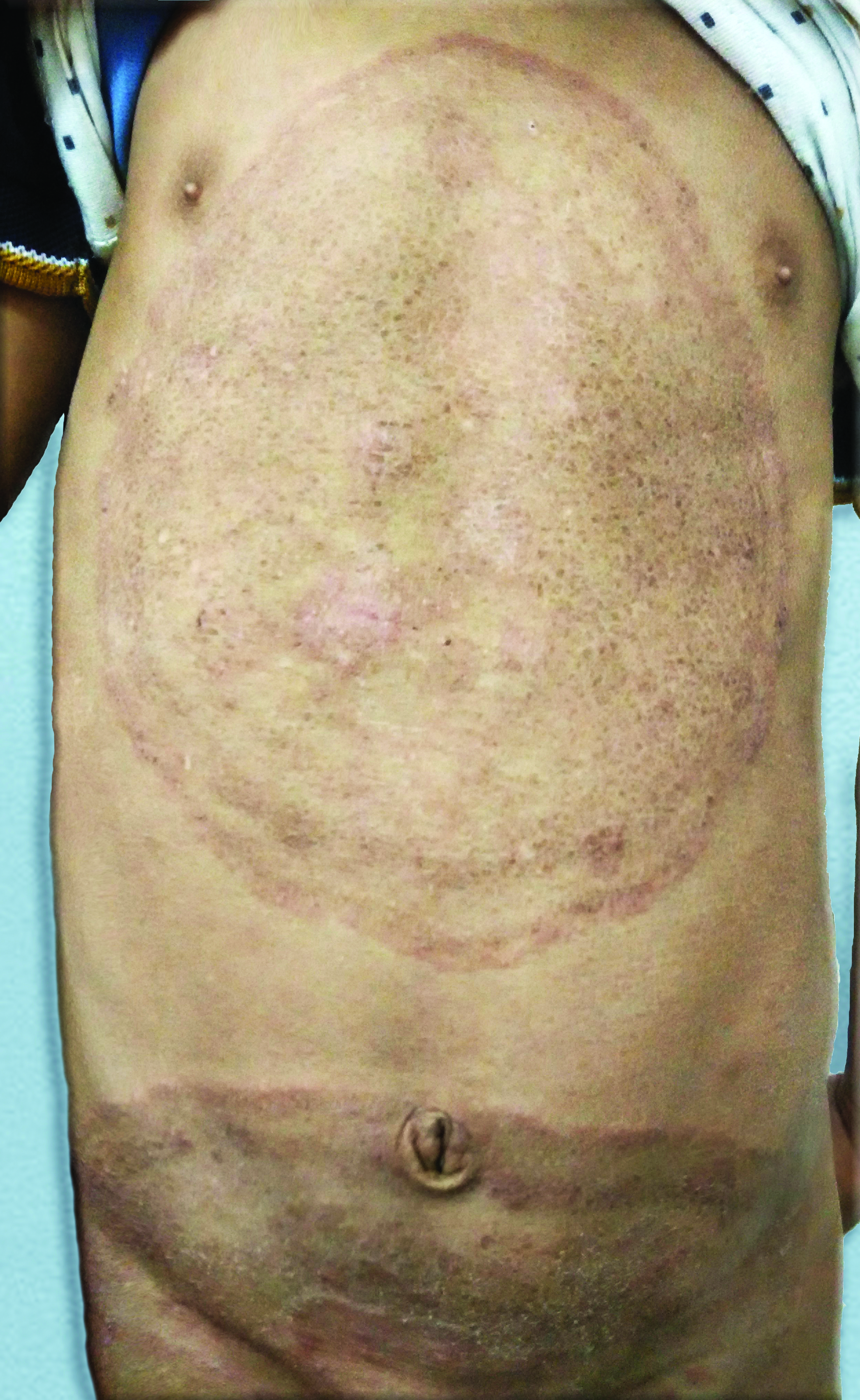
- Giant concentric rings of tinea pseudoimbricata over the torso.
Tinea pseudoimbricata resembles tinea imbricata, but has no geographical predilection and is caused by dermatophytes other than Trichophyton concentricum. It is a rare presentation of steroid-modified tinea labelled as tinea incognito/tinea atypia. Inadvertent use of topical corticosteroid drugs causes this altered morphological presentation[1]. Aggressive treatment with both oral and topical antifungal agents is warranted in tinea pseudoimbricata. To avoid any relapse in the future, the clinical cure should always be confirmed by the relevant tests for confirming mycological cure.
Declaration of patient consent
Patient’s consent not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Tinea incognito in Korea and its risk factors: Nine-year multicenter survey. J Korean Med Sci. 2013;28:145-51.
- [CrossRef] [PubMed] [Google Scholar]





